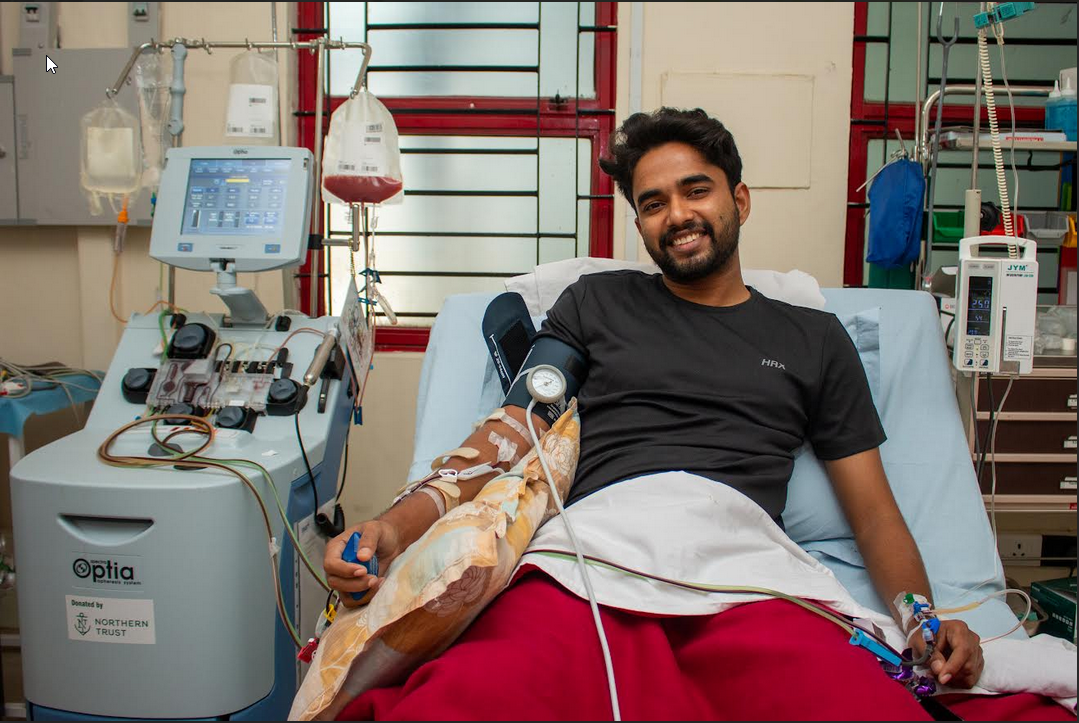
For medicines to work safely, it’s vital to have strong systems in place to report any undesired side effects or “adverse drug reactions“.
The most important aspect of drug safety monitoring is reliable, real-time information. Health-care professionals (physicians, pharmacists, nurses, dentists) are best placed to report suspected adverse reactions as part of patient care.
Patients also have a critical role in getting the right information to authorities and should refer to their medical practitioner as soon as they detect unwanted symptoms or reactions. Both health professionals and patients should report these even if they are doubtful about the precise relationship between the given drug and the reaction.
Most adverse reactions are preventable
Many undesired drug reactions may be due to factors independent of the medicine. For example:
- incorrect diagnosis of the patient’s medical condition;
- prescription of an inappropriate drug or incorrect dosage of the appropriate drug;
- an undetected medical, genetic or allergic condition that may cause a patient reaction;
- self-medication with prescription medicines;
- not following instructions for taking the medication;
- interactions with other drugs (including traditional medicines) and certain foods.
But risks may also occur because a medicine’s composition and ingredients do not meet required standards, causing them to be ineffective and even hazardous; or because the medicine is counterfeit, with no active ingredients or inappropriate ingredients.
Assessing medicines before and after they reach patients
Before medicines or vaccines are made widely available in countries, they have rigorously tested inpatient and healthy volunteers respectively to discover how well they work for a defined disease and how safe they are. But to get a comprehensive picture of a product’s safety, it is important to keep watching how it works once it is widely used in a population.
This requires careful patient monitoring and further scientific data collection by organized local, national and international agencies.
Drug safety during the COVID-19 pandemic
International drug safety monitoring is particularly important during global epidemics such as the current COVID-19 pandemic, and even more so when there are no proven vaccines or medicines for the disease. As new COVID-19 vaccines and treatments become available, health-care professionals and patients will need to be actively engaged in monitoring the effects of these novel products and reporting any potential adverse reaction. By analyzing reported reactions, national medicines authorities can take the necessary measures for safer use of the drugs, scientists can assess the data and, if needed, international networks can be activated to address the problem.
WHO’s role in making medicines safer
WHO promotes global drug safety through its Programme for International Drug Monitoring, which supports countries to develop sound pharmacovigilance policies, organizes hands-on training and workshops, and establishes networks for information sharing.
An important role of the programme is to strengthen national reporting systems and their contribution to VigiBase, the global WHO database for adverse drug reactions, managed by Uppsala Monitoring Centre in Sweden, and to identify possible links between the use of a drug and adverse reactions. When signals of drug safety problems emerge through the database or other sources, WHO and Uppsala Monitoring Centre share new information on serious adverse reactions with all WHO Member States.
A recent key WHO development is the introduction of a mobile application called “Med Safety”, jointly launched in nine countries* with Uppsala Monitoring Centre and the UK Medicines and Healthcare products Regulatory Agency. The app enables health-care professionals and patients to report suspected adverse reactions directly to the national authorities’ database. WHO is preparing to roll out the app in more countries once a COVID-19 vaccine becomes available.
 For medicines to work safely, it’s vital to have strong systems in place to report any undesired side effects or “adverse drug reactions“.
For medicines to work safely, it’s vital to have strong systems in place to report any undesired side effects or “adverse drug reactions“.







.jpg)
.jpeg)










.jpeg)



.jpg)






.jpg)